I woke up around 7:30am on the morning of Thursday, April 19 with my water breaking. Â It was a really weird feeling — like peeing without having any control over it. Â I went back to bed and figured if it was “something important,” it would still be going on in another hour. I knew Peter had gone to bed super late after working at Ice Oasis until 5am, so I wanted to let him sleep as long as possible. Â At 9:30am, I woke up again and still felt the trickling, so I got up and called the OB office. Â Not terribly surprisingly, they told me to come right in.
I woke up Peter (who was very good-natured about it) and we made our way out of the house. Â I brought along my hospital bag “just in case” even though I thought they might just send us home…but I also knew that I was in complete denial about the water breaking since that would mean that, holy crap, I’d have to birth a baby.
Dr Sukhdeo got me onto the exam table and as soon as I shifted position for him to look, a bigger gush of fluid came out. Â That pretty much sealed the deal and he told us we’d have the baby that day. Â I maintained my utter denial.
Since I wasn’t having any painful contractions at all — just leaky! — we decided to get lunch at Pizza My Heart on our way to the hospital. Â Yum pepperoni pizza slice!
We drove to Lucile Packard Children’s Hospital and were admitted immediately. Â I was put into a Labor & Delivery room and introduced to our nurse, Kirsten. Â Dr Karl came in a little while later to say she’d be delivering our baby — I had only met her briefly previously, but she had delivered my coworker Brian’s daughter. Â When Brian and I had compared LPCH notes back at my work baby shower lunch, he’d had only good things to say about her.

Dr Karl explained that we’d want to start an IV for antibiotics since my Group B strep test wasn’t back yet. Â That was fine by me. Â She also wanted to start Pitocin, which I wasn’t as OK with. Â She left and Peter and I discussed it; I was concerned that Pitocin would lead to a more painful labor and therefore an epidural, but Peter convinced me that it was already 2pm — I wasn’t having any contractions at all, really, and we should get the party started if I wanted to have the baby while I still had any energy left. Â So I begrudgingly agreed to the Pitocin.
At 3pm, Kristen started me on the ampicillin and Pitocin (level 1).
At 4pm, Kristen raised the Pitocin up to level 2. Â I still wasn’t feeling anything at all and was essentially sitting around the L&D room waiting to hurt. Â Peter had run back to the house for the car seat and some stuff for himself; I was texting friends and family and just puttering around on the internet.
Shortly after 4pm, my low back started to hurt during contractions. Â It felt like a lesser version of the back pain from my disc injury.
At 4:30pm, Kristen raised the Pitocin level to 3. Â She wanted to increase it more, but I convinced her that I was already starting to feel the contractions and I wanted to see how this progressed before we just ramped up the medication to crazy levels.
By 5:15pm, I was definitely having back pain with contractions. Â This was around the time I stopped taking notes on my laptop, too. Â I don’t know how far apart the contractions were or how dilated/effaced I was — since I was already at L&D and getting underway, no one really needed to know any details.
Within a couple of hours, I was in some pretty serious pain (we’re talking an 8 or 9 on the Hyperbole and a Half pain scale, and I have a high tolerance). Â I tried to move around and change positions like they suggested in our Childbirth Prep class, but the only thing I could really do at all was curl up on my right side and grab onto the bedrail for dear life. Â I kept trying to burrow my head into the bedrail, which would occasionally push a button and make the bed move up or down. Â I couldn’t stand to be touched at all aside from a cold washcloth on my forehead. Â I just kept doing the breathing we’d learned in class — three short exhales and a long exhale. Life was not really very good.
I started seriously contemplating wanting an epidural. Â I don’t know who suggested it, but someone thought I should try Fentanyl first. Â The anesthesiologist came in (a very nice man who unfortunately probably gets screamed at all day) and they probably asked me some questions that I don’t have any chance at all of remembering. Â I felt better immediately after getting the first dose of Fentanyl — it didn’t make the pain stop but I could rest between the contractions. Â I would basically fall asleep until the next one started up again. Â I entered this strange state of druggie woozy coma OH GOD THE PAIN OH GODÂ druggie woozy coma, lather rinse repeat.
This went on for another couple of hours until I’d had the maximum three doses of Fentanyl (each one was good for up to an hour, I think). Â The final dose wore off shortly after 10pm and I was told I could start pushing at 10:30pm.
True to their word, I started pushing at 10:30pm. Â I didn’t really know what I was doing and it took me a while of misery to figure out which muscles I need to engage and which to simultaneously relax. Â Without the Fentanyl, there was no down time between the contractions and by the time the next one started up, I’d forgotten how I’d done the push the previous time. Â Peter, Dr Karl, and the nurses had to remind me to relax my hips every 90 seconds for 2 hours.
Pushing was a huge pain, and not just for the obvious reasons. Â I was getting very tired and discouraged and I felt like I just wasn’t pushing “right”. Â Everyone would get excited and tell me “she’s moving!” and then I’d stop pushing and she’d kinda sneak back up. Â This is normal, of course, but it was still so demotivating. Â I wound up pushing for almost 2 hours and it wasn’t until the last 10 minutes or so that I felt like I was being even a little bit productive.
At the very end, I could tell we were close because Peter got very excited and told me he could see her head right there and that it would only be a couple more pushes before she was out. Â I don’t have a memory of how those last few pushes felt differently than the previous ones; I remember a vague sense of “different” but I couldn’t describe it. Â I guess they just felt more productive. Â I remember seeing Dr Karl slip on something that looked like a blue hazmat suit (their “catching gear”), which was finally motivating — even in pain, I realized she wouldn’t be doing that if the baby weren’t mere moments away!
One or two more pushes and suddenly everyone was very very excited and Kira was born at 12:16am. Â She was placed on my stomach and I vaguely remember Dr. Karl asking Peter if he wanted to cut the cord (I don’t recall this at all, but he did do the cut) and then they whisked her across the room to the little mini incubator to weigh her and make sure she had the right number of heads and legs and eyeballs. Â I remember hearing her cry out for the first time.
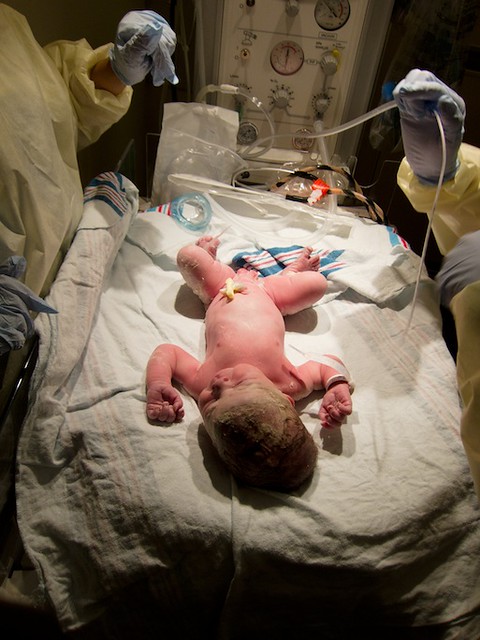
Peter stood with her and the pediatric team (I have absolutely no recollection of that SWAT team entering the room) while Dr Karl finished up with me. Â I delivered the placenta, which was pretty painful as well…but Dr Karl reminded me that I was done once that was out, so I was extra motivated to push that time! Â It came out onto the table and I thought it was so cool that I called out for Peter to come take a look. Â I didn’t have a great view but Dr Karl showed it to Peter and showed him how the amniotic sac had held Kira. Â He said it was pretty neat.
I had an internal first degree laceration that needed one stitch, so basically no tearing at all. Â Woohoo! Â Dr Karl stitched that up, which was not comfortable…but at that point anything that wasn’t a baby’s head was practically relaxing.
Kira was cleaned off at this point and wrapped up and handed back to us. Â And thus we became a family.

Birth stats:
Kira Brooks Bierman
Born 12:16am on Friday, April 20, 2012
6 pounds, 9 ounces
19″
Apgar scores: 8 at 1 minute, 9 at 5 minutes